The main problem with this test is the possibility of either “false positives” or “false negatives”. In the former, a test may appear to indicate an abnormal test, but subsequently no real abnormality shown. In the latter, which is less common, no abnormality may be shown, and subsequently a real underlying problem is identified. This latter problem is more likely in patients who were unable to exercise sufficiently. In some cases, a test may be “equivocal”. That is to say that there may be minor ECG changes observed that are not diagnostic of ischaemia. This can present a quandary, but depending on the clinical symptoms, the degree of suspicion either increased, or the patient reassured. The accuracy of the test is about 70-80% and does depend on how well the patient can perform. The main value of the test is that it is prognostic. If a patient has identified disease, but can perform well on exercise, their prognosis will be good.
In patients who cannot exercise, alternative tests include nuclear imaging, stress echocardiography, or direct anatomical visualization using cardiac catheterization or CT angiography. 
Myocardial Perfusion Scan (by Nuclear Imaging):
This is another non-invasive means of investigating patients with suspected angina. In this case as with exercise testing, it is a functional test, where the arteries are not directly visualized. Instead, a small amount of radioactivity is injected into a vein. It is taken up by heart muscle and causes the heart to “glow” on a screen. The test is performed under resting conditions, and under stress (exercise) conditions. In this way if under resting conditions there is an underlying previous total blockage from a previous heart attack; that section will not “glow” on the screen, and appear as a “black hole”. In the second part of the test under exercise conditions, the heart is stressed either physically using a bicycle or treadmill test, or chemically stressed using medication to speed up the heart. If the heart appears normal under exercise conditions, but under stress if a “black hole” appears; this would signify a reduced supply to a section of heart muscle. This would often suggest an anatomical narrowing. Depending on the size of the anatomical narrowing, the prognosis can be determined.
The resting and stress components of the test are set about 6 hours apart, so from a practical point of view take up half a day of patient time. The test very rarely misses any underlying ischaemia, but may falsely identify an area of ischaemia. That is to say, show up a black hole that is subsequently shown to be normal. That is the main limitation of the technique, but if patients are well selected (e.g. not too overweight, etc) then an accurate result should be anticipated.
In cases where a “black hole” is identified under exercise conditions, then a decision would be made as to whether to proceed to undergo cardiac catheterization for anatomical confirmation. If there is a minimal degree of ischaemia (say 10% or less), or the test is normal the patient can be reassured. 
Stress Echocardiography
This is also a functional and non-invasive test used commonly to identify ischaemia. In this test conventional ultrasound of the heart (see echocardiography) is used to identify that the heart muscle contracts in a uniform manner. If there has been a previous heart attack, then this would show up on the scan as a section of heart muscle that is thinner than normal and does not contract well (so called wall motion abnormality). In the absence of this, if the heart is chemically stressed with adrenaline like substances, the heart should contract more vigorously. However if there is a narrowing of a coronary vessel, under exercise conditions or chemical stress, this would reflect itself in reduced muscle contraction. The area and degree of wall motion abnormality would signify the severity of ischaemia.
The test takes about 45 minutes to perform. Not everybody is suitable to have the test performed, as the test depends on the heart being well visualised at rest. About 10-15% of patients are not well visualized with this technique. However, recent advances using additional chemicals to better “see the heart” have improved the situation. A negative test provided the heart has been stressed sufficiently, excludes the likelihood of significant abnormality and is thus prognostic. If a significant wall motion abnormality is seen, then this would indicate a need to pursue cardiac catheterization.
The main limitation of this technique is that although a sensitive test, it may not be as specific, and have false positives; i.e. show abnormalities that may subsequently be normal. The main problem is that the test not infrequently shows equivocal changes where it may not clearly identify whether a problem truly exists. In such cases additional testing may be necessary. 
Cardiac Catheterisation
This is an invasive technique that involves intubating the coronary arteries directly to investigate patients with significant cardiac sounding chest pain. Patients are fully awake during this procedure as it is relatively painless. Sedation however can be requested on demand. The procedure generally takes less than 30 minutes. Local anaesthetic is administered at the top of the leg near the femoral artery.
Alternatively the artery in the wrist can be used. A hollow needle is passed into the artery via a small hole (3 mm). A guidewire is then passed through the hollow needle into the arterial circulation. This acts as a railway line to then pass a short plastic tube into the artery, the size of a drinking straw. It has a bobble on it which acts as a non-return valve to prevent blood leaking out. It is through this plastic tube that longer tubes are passed up the leg artery (or arm artery) to the heart. The X ray camera is on the outside and is used to guide the longer tubes (called catheters) to the arteries of the heart. A small amount of dye is then injected into the artery and pictures are taken with the camera. Different pictures are taken at different angles to get complete visualization of the coronary arteries. In addition, pressure measurements can be made to assess the significance of valve narrowings too.
This test is not however without risk. It is undertaken judiously when the benefit of performing the test and assessing the arteries outweighs the risk of performing it. We quote overall risks of either having either a stroke or a heart attack as 1 in a 1000. It is a small but not insignificant risk, hence the need to carefully select who would benefit from it.
The result of the cardiac catheter test could reveal that the arteries are normal, and thus the patient can be reassured. The test may also reveal that there may be mild narrowing of the arteries, but no intervention is required. This would indicate that a narrowing process (called atherosclerosis) has begun, but if risk factors are treated aggressively, and aspirin added, the condition will not deteriorate, or even can be reversed. A critical lesion would be identified as a narrowing of about 70% of the diameter of the vessel or more. Bear in mind that the degree of narrowing does not correlate with the chance of a heart attack.
All you can say is that the degree of narrowing correlates with the chance that angina is likely to be due to the narrowing. If one or more narrowings deemed significant (i.e. usually greater than 70% narrowing) then a decision can be made whether to treat it with angioplasty or surgery. Symptoms are the main guide to treating the narrowings. So despite the presence of narrowings, if medication relieved the angina, perhaps then no intervention would be necessary. If however symptoms persisted despite medication, or that medication was not tolerated, then intervention would be appropriate. 
Calcium Scoring
This non-invasive technique involves a quick scan using CT scanning to measure the calcium content within the coronary arteries. It cannot tell whether there are narrowings within the arteries, however the amount of calcium accumulation has been shown to be prognostic. It is an accurate means of identifying cardiovascular risk.
Its main application is in determining patient risk of developing coronary disease. Thus it is not an appropriate test for those with symptoms. In patients with risk factors for coronary disease, the finding of significant calcification may further stratify patients to be more aggressively treated for conditions such as an equivocal cholesterol elevation, diabetes, smokers, hypertension, or indeed those with a strong family history. In such cases, the finding of significant calcification may indicate a greater need to treat a patient more aggressively.
The question posed by many is how to investigate patients with a high score. The higher the calcification (measured with the Agatston score) does indicate a greater risk to the patient. Generally there is no need to investigate patients further, unless the patient develops symptoms. The mainstay of treating such patients is to treat risk factors aggressively, and prescribe aspirin and statins. 
Cardiac CT Angiography
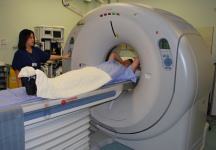 This is a non-invasive test to diagnose coronary disease, and usually also involves a calcium score. It is an alternative to cardiac catheterization that is without the possible risk of either a heart attack or a stroke. In recent years, the dose of radiation has been reduced substantially. However, in young women in particular, one should try and avoid the risks of radiation exposure. Patients need to be carefully selected to maximize good image quality. In very large patients or those with fast irregular heart beats, then poor imaging may prevent good visualization. Ideally patients should have their heart rates at around 60 beats per minute. This is usually achieved by pre-treating patients with heart rate lowering drugs for a few days prior to the procedure, or just before the test. The procedure itself takes about 15 minutes. Most of this is preparation which involves a small injection and making some measurements. The actual scanning time is only about 7 seconds. The scanner looks like a giant “Polo Mint”. The patient is on a couch that will move forward through the Ring like structure, so there is no chance of becoming claustrophobic. After the scan, the patient can hop off the couch and go home. This is a non-invasive test to diagnose coronary disease, and usually also involves a calcium score. It is an alternative to cardiac catheterization that is without the possible risk of either a heart attack or a stroke. In recent years, the dose of radiation has been reduced substantially. However, in young women in particular, one should try and avoid the risks of radiation exposure. Patients need to be carefully selected to maximize good image quality. In very large patients or those with fast irregular heart beats, then poor imaging may prevent good visualization. Ideally patients should have their heart rates at around 60 beats per minute. This is usually achieved by pre-treating patients with heart rate lowering drugs for a few days prior to the procedure, or just before the test. The procedure itself takes about 15 minutes. Most of this is preparation which involves a small injection and making some measurements. The actual scanning time is only about 7 seconds. The scanner looks like a giant “Polo Mint”. The patient is on a couch that will move forward through the Ring like structure, so there is no chance of becoming claustrophobic. After the scan, the patient can hop off the couch and go home.
Most of the application of CT angiography involves visualizing the coronary arteries. It is accurate in about 94% of cases which is excellent (bearing in mind that no test is 100% accurate). Unlike cardiac catheterization which only looks at the inner vessel, this technique visualizes the whole of the vessel wall. As coronary narrowings usually begin in the wall of the vessel, they would not be seen during cardiac catheterisation until they encroach inwardly. With CT however the process can be detected at a far earlier stage and treated.
In addition to the arteries, the rest of the cardiac anatomy can be seen. Holes in the heart, abnormal thinning or thickening of heart muscle can be detected. The pericardium, not at all seen on echocardiography can be seen for potential pathology.
One major application of CT angiography is in evaluating other potential causes of chest pain at the same time. The lungs are seen for potential clots or infection that can cause chest pain. Diseases of the aorta such as aneurysms or tears (dissection) can be excluded. Pericardial thickening can be identified as a cause of chest pain. Finally gastric reflux or a hiatus hernia can be detected simultaneously. In summary, for patients with unexplained chest pains that have not been diagnosed by previous tests, this provides a fairly definitive means of getting to the bottom of the problem. 
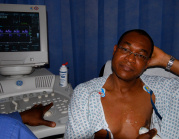
Echocardiography
This is a painless non-invasive imaging technique. It provides information on heart function and the size of the chambers, valve function, and may reveal evidence of heart damage. It is performed at the bedside with a probe placed on the chest. 
Transoesophageal Echocardiography
This is a more detailed invasive technique for viewing the heart and its structures more closely. It is particularly useful in assessing the degree of heart valve function (especially the mitral valve), and diagnosing “holes in the heart”. It also has a major application in excluding or diagnosing clots (thrombus) as a cause of mini-strokes. Unlike normal echocardiography, this is an invasive technique. It takes about 30 minutes to perform. Patients may be sedated slightly, and have the back of their throats anaesthetised. A mouth guard is inserted to prevent the patient biting through the tube.
A tube about 1 cm in diameter is passed to the back of the throat and the patient encouraged to swallow the tube down. It is a mildly uncomfortable procedure quite similar to Endoscopy, but generally well tolerated. When the tube is in the oesophagus, the heart can be evaluated using ultrasound. It is a safe procedure, and complications such as traumatising the oesophagus or displacing any teeth are easily avoided by being careful. 
Ambulatory monitoring of ECG
We regularly perform this test to gain a more continuous evaluation of symptoms of palpitations or dizziness. If symptoms are daily, then a 24 hour ECG can be performed. For symptoms occurring at least weekly, a 7 day monitor can be used. The difficulty is in patient’s whose symptoms are sporadic and occur infrequently. Certain devices such as a Zio monitor can be worn for 2 weeks. For less frequent episodes, an implantable ECG loop recorder can be inserted unobstrusively under the skin under local anaesthetic and remain in place for up to 2 years. Patient driven appliances with computer or phone Apps can be used. Unfortunately, many of these devices are unvalidated, although the AliveCor device is now recommended.
If the symptoms last long enough, I usually provide a patient with a “To Whom it May Concern” letter, explaining that if the patient presents with symptoms, to kindly perform an urgent ECG on arrival in an emergency department. I give this letter to the patient and tell them to go promptly to the Accident and Emergency Department (if out of hours), or to the Cardiac Department during working hours to obtain an ECG.
Ambulatory monitoring of blood pressure
This is performed to gain a more continuous evaluation of blood pressure in “real life conditions”. This is quite useful in excluding artificial elevations in blood pressure – so called “white coat hypertension”. In addition for patients that have a labile blood pressure, it can evaluate whether there are significant episodes of elevated blood pressure. We normally expect blood pressure to be low, unless the patient is a night shift worker. The essential measurement is the average daytime pressure as an indication of sustained hypertension. Overall, elevated 24 hour blood pressure correlates with the risk of complications and should be treated. 
Cardiac MRI
This is also a non-invasive test that images the heart. There is no radiation involved, but patients need to lie in a large cylinder. Claustrophobic patients sometimes may have difficulties being in the chamber. I myself am claustrophobic but have been in the scanner three times. Infact, most claustrophobic patients do tolerate the procedure, as there is usually enough space around the scanner. In addition, the patient’s head is at the top end and one can sometimes see outwards.
The test is used to clearly define the anatomy of the heart, even in patients with poor visualization with echocardiography. The test is very good at accurately measuring heart function. If there are narrowings or leakages of the heart valves, then these can be accurately assessed with this technique. Another major application is in the assessment of heart muscle itself. If there are concerns whether heart muscle is permanently damaged or not, this technique with a contrast agent offers the best method of assessment. This is applicable in situations where there is perceived damage to heart muscle and a decision needs to be made as whether to revascularise the heart. If the scan reveals only partial heart muscle damage, then there would be great benefit . 
|